Every aspect of our daily lives, from our mood on a Monday morning to how well we sleep on a Friday night is being governed by our endocrine system, the system responsible for the regulation and production of hormones. This fragile system of balance can easily be disrupted by a number of things, the key of which are endocrine disruptors (EDs). EDs are chemicals or other exogenous factors that disrupt the endocrine system’s ability to function healthily, resulting in adverse health effects such as increased cancer risk & growth impediments. From the stories of those with hormone-related disorders to nutritional research, there is little doubt that EDs are bad for us, so why are they still found within the products on supermarket shelves? Why does regulation against EDs remain at a standstill for regulatory bodies such as the EU? Unfortunately, the situation is far less black and white than it seems, due to the intricacies that surround both the policy making process as well as the composite nature of the data gathered.
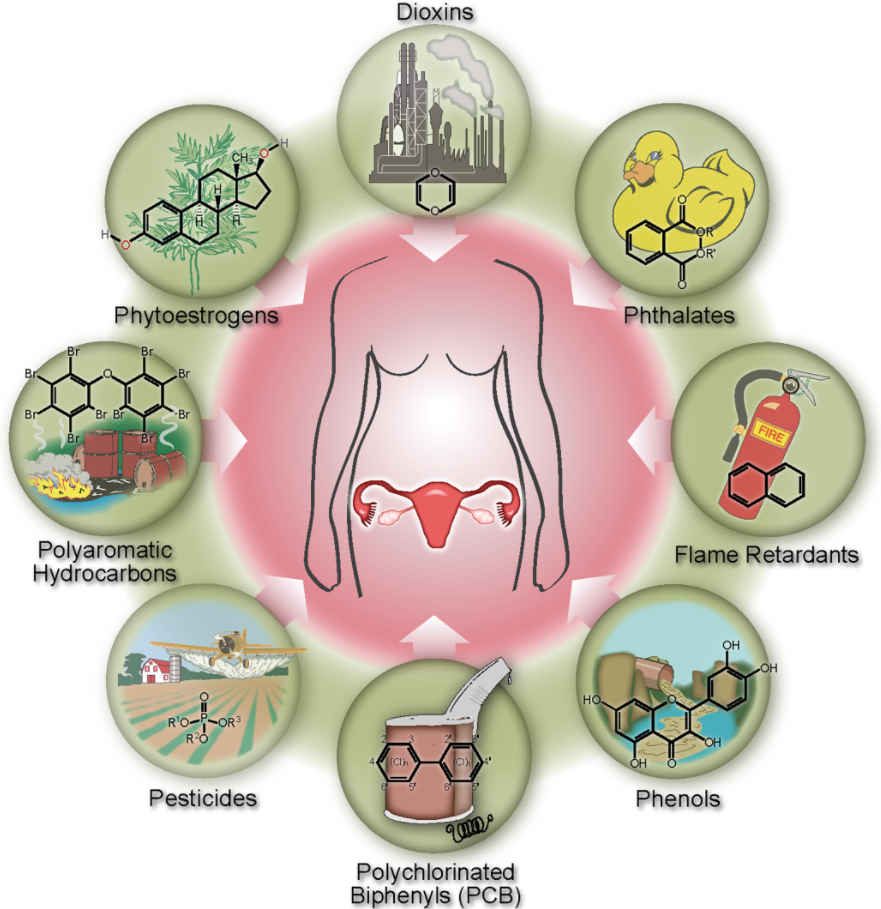
Image: Examples of Endocrine Disruptors
Firstly, a fundamental reason as to why progress has been slow is the lack of public pressure. Policy changes are largely shaped by public perception and interest. Since democratic governments do what they can to remain in power they are incentivised to prioritise what the public wants in order to garner votes. In the case of EDs, it is a health topic that remains virtually unknown to the general public. This is evidenced in both attitudinal surveys and qualitative studies. In a focus group study done in Northern Ireland, participants were completely unaware of the term, unless they were personally victims of hormone-related disorders or possessed prior education in the area. The lack of awareness on the issue disincentivises policy-makers to concentrate efforts on this policy area, when time and effort could be better focused on gaining popularity through advancement on more hot-topic policies.
Beyond the lack of will to act, there is also a certain level of “inability” to act due to conflicting scientific findings. This is a result of difficulties in both conceptualisation (defining key terms) and operationalisation (measuring the severity of effect). The debate on EDs remains complex due to several focal issues that have to be addressed before science can make any headway in this area.
Conceptualisation
Even the term “endocrine disruptor” is contentious. The definition by the World Health Organisation (WHO) is “an exogenous substance/mixture that alters function(s) of the endocrine system and consequently causes adverse health effects in an intact organism …”. While this definition may seem specific, terms such as “function of the endocrine system” are highly disputed. For example, some researchers define this as any change in the hormonal concentration of the blood. Hence, something as simple as a bar of chocolate would be seen as an ED, since it increases insulin (hormone) secretion. However, would such a definition be useful?
In comparison, the Endocrine Society defines EDs as “ an exogenous chemical or mixture of chemicals that interferes with any aspect of hormone action”. Following this definition, an ED would instead be something that changes the way the organ responds to the stimulus such as by blocking the ability of insulin to increase or reduce glucose levels. By focusing on the functionality of the hormones rather than the endocrine system itself, the definition of an ED thus becomes far stricter.
Operationalisation
The data pool grows ever murkier when we take into account the difficulty of measuring hormonal disruptions, especially given the fact that EDs usually do not occur singularly. I.e., your food may contain more than one type of ED, leading to what scientists define as the “cocktail effect”. Meaning that while a certain chemical’s level within the product may be too minute to cause harm, its exposure to other EDs (at equally low levels) within the product may actually result in more potent adverse effects. Given these circumstances, it is difficult to pass blanket policies over what precisely counts as unhealthy ED levels. Each product is likely to have to be individually investigated, requiring immense effort, time and money on the part of regulatory bodies.
In summary, these series of confusions and complexities have resulted in conflicting reports and expert opinions. Confusion and conflict are so rampant in the field that it has led to an impasse in the progress of policy creation on the subject matter, For example, the WHO’s 2010 ED report provoked both a critical editorial and review in disagreement. Ultimately, evidence-based policymaking is not as clear-cut as the way it is in evidence-based medicine, due to the subjective nature of the policy-making process as well as the complexity of the data collection and interpretation. In order for us to make policy progress, it is crucial to mobilise public awareness and support for change, alongside creating consensus within the scientific community.
Note: This article gives the views of the authors, and not the position of the Social Policy Blog, nor of the London School of Economics.





Interesting! Never knew these things are entering our body
Nice writing